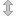Healthcare is a fast-paced industry, and the importance of medical billers and coders cannot be underestimated. Medical billing and coding are an in-demand career that allows hospitals and healthcare offices to run efficiently while providing patient care.
What do Medical Billers and Coders Do?
Medical billing and coding play an important part in connecting health care providers, insurance companies, and patients. General duties for medical billers and coders include reviewing patient information, assigning appropriate diagnosis and procedure codes for patient care, statistical tracking, and billing purposes.
Medical billing and coding involve identifying diagnoses, treatment, medical tests, and procedures found in clinical documentation and then transcribing patient data into standardized codes to bill government and insurance companies for physician reimbursement.
Become a Medical Biller and Coder
For a medical coding and billing career, you need to complete online medical coding and billing training and successfully pass the certification exam. Online degrees allow students to study at their own pace and at times that are convenient for them. Lectures and class materials are typically available on a 24-hour basis online so that students can study and access the material anywhere, at any time.
Medical billing and coding degree programs typically have three levels: diploma or certificate program, associate degree, or bachelor's degree. Diploma and certificate programs solely focus on the professional skill needed to graduate quickly and start working.
Below are five things you will learn when you get a degree in medical billing and coding:
- Responsibilities of a Medical Biller and Coder – medical billers and coders are responsible for taking patient files and translating them into billable codes and notes. Translating codes allows medical practices to correctly bill patients and insurance companies. Specific codes have been assigned to various procedures and diagnoses, which the medical biller and coder use to track each patient's information.
- Health Insurance and Reimbursement – medical billers and coders will explore reimbursement and payment methodologies that apply to healthcare-related to relevant forms, processes, practices, and health information professionals' roles.
- Classifying Medical Data – you will learn the proper abstract, classify, and code medical data while ensuring data quality and integrity.
- Process Information – in a medical billing and coding program, you will learn to compile codes, categories, calculations, tabulations, and audits and verify information and data.
- Current Procedural Terminology – study the principles and guidelines for using the current procedural terminology system for reporting healthcare services and physicians, including non-inpatient procedures.
What Jobs Can You Get with a Degree in Medical Billing and Coding?
Graduates of a medical billing and coding degree program open the door to various medical fields' careers. Generally, medical billing and coding graduates will find work as office staff of healthcare facilities. Here are some professions that a graduate who has completed medical billing and coding training can expect to get:
- Medical Record and Health Information Technicians – responsible for managing and organizing patient data. These technicians record the proper coding for billing and statistical tracking.
- Medical Assistants – assist nurses and doctors with patient care and administrative duties. Some of their tasks can include scheduling appointments, recording patient information, and taking patient vital signs.
- Medical Transcriptionists – responsible for listening to a physician's voice recordings and transcribing information into a written report. They also might enter reports into electronic record systems.
Conclusion
If you are interested in medical billing and coding, you need to understand codes and current healthcare laws. A medical biller and coder needs to keep knowledgeable by attending continuing education opportunities.
Medical billers and coders should be analytical and critical thinkers who can uncover the correct codes and problem-solve to ensure they are billing correctly and no details are overlooked.
 icons at the top right corner of the subsection.
icons at the top right corner of the subsection.